Achilles Tendinopathy Rehab: What Actually Works?
Achilles Tendinopathy Rehab: What Actually Works?
Quick Answer
The most effective rehab for Achilles tendinopathy is progressive, heavy, slow loading of the tendon — not just basic heel raises. Research suggests that loading at 70–90% of your maximum strength, performing slow 6-second repetitions, and progressing through isometric → heavy slow resistance → plyometrics produces the best tendon adaptation. The key is not just doing exercises, but loading the tendon correctly and progressing based on tolerance.
Why Achilles Tendinopathy Is Often Mismanaged
Many people with Achilles pain are told to:
- Stretch more
- Rest completely
- Do a few bodyweight heel raises
While heel raises are a starting point, the dosage and progression matter far more than the exercise itself.
Tendons respond to mechanical strain. If the load is too light, the tendon does not adapt. If the load is too aggressive, symptoms flare. The goal is controlled, progressive strain that stimulates collagen remodeling.
Whether you're a Boulder runner training for a marathon, a CrossFit athlete, or someone who developed pain from a sudden activity increase, your rehab should be structured — not random.
The 4 Variables That Matter Most in Achilles Rehab
Recent expert consensus in sports medicine research identified several key parameters that influence outcomes in Achilles rehabilitation. Here’s what matters in practical terms.
1. Intensity: How Heavy Should You Load?

Tendon remodeling is strain-dependent.
To stimulate structural change, loading typically needs to reach 70–90% of your 1 repetition maximum (1RM).
That means:
- Bodyweight alone is often not enough.
- Added load (dumbbells, barbell, Smith machine, or weighted vest) is usually required.
- Athletes may tolerate higher loads earlier.
- Sedentary individuals need a gradual ramp-up.
Clinical rule:
If your heel raises feel “easy,” they’re probably not stimulating adaptation.
At Boulder Sports Clinic, we often measure calf strength and use that data to determine appropriate loading instead of guessing.
2. Tempo: Move Slow to Remodel Tissue

Tendon response depends on time under tension.
Experts recommend approximately:
- 3 seconds up
- 3 seconds down
- ~6 seconds total per repetition
Fast, bouncy reps reduce effective tendon strain and shift work to elastic recoil rather than tissue remodeling.
Early rehab focuses on slow, controlled loading. Later stages may incorporate faster movements to restore power and sport readiness.
3. Sets and Reps: Volume Progression
There isn’t one perfect prescription, but most programs follow this progression:
Early Phase
- 3–4 sets of 12–15 reps
- Moderate load
- Controlled tempo
Progression Phase
- 3–4 sets of 6–8 reps
- Higher load (approaching 70–90% 1RM)
- Maintain slow tempo
As load increases, total reps often decrease to allow recovery.
Pain Monitoring Guidelines
A practical framework many clinicians use:
- Pain during exercise ≤ 5/10
- No significant next-day flare-up
- No disruption to sleep
Mild discomfort during loading is often acceptable. Increasing stiffness or worsening pain the next morning signals overload.
4. Contraction Type: It’s Not Just Eccentrics
The classic Alfredson protocol emphasized eccentric-only loading. We now know eccentric loading is effective — but not superior to other types when total load is matched.
A well-structured program includes:
Isometrics (Early Phase)
- Holding heel raise positions
- Helpful for pain modulation
- Useful in reactive or highly irritable tendons
Slow Isotonic (Concentric + Eccentric)
- Heavy slow resistance
- Builds true tendon capacity
- Core phase of rehab
Plyometrics (Late Phase)
- Jumping, hopping, bounding
- Restores elasticity and sport readiness
- Essential for runners and field athletes
Special Consideration: Insertional Achilles Tendinopathy
Insertional cases (pain at the heel bone attachment) require additional care.
Excessive dorsiflexion increases compressive load between the tendon and calcaneus.
Early phase adjustments:
- Avoid dropping heel below neutral.
- Perform raises on flat ground rather than off a step.
Later phase:
- Gradually reintroduce full dorsiflexion range as tolerance improves.
This is one of the most common reasons people fail rehab — they unknowingly overload the insertion early.
Who This Is For
This approach is ideal for:
- Runners with mid-portion Achilles pain
- CrossFit athletes or lifters with tendon stiffness
- Active adults with gradual-onset Achilles pain
- Patients who have plateaued with basic rehab
This approach is not for:
- Acute tendon ruptures
- Systemic inflammatory conditions without medical clearance
- Severe insertional cases not yet tolerating load
How We Decide Treatment in Boulder
At Boulder Sports Clinic, we don’t automatically prescribe the same protocol to every Achilles case.
We evaluate:
- Calf strength asymmetry
- Tendon thickness and irritability
- Running or training volume
- Ankle mobility and dorsiflexion tolerance
- Hip and foot mechanics
From there, your program may include:
- Progressive heavy slow resistance
- Gait analysis for runners
- Shockwave therapy for stubborn tendinopathy
- Dry needling or soft tissue therapy to address calf stiffness
- Chiropractic care if joint restrictions are contributing to altered loading
Exercise remains the foundation — but supporting factors often influence recovery speed.
How We Treat Achilles Tendinopathy at Boulder Sports Clinic
At Boulder Sports Clinic, exercise is the foundation of Achilles rehabilitation — but it’s rarely the only piece. We combine progressive tendon loading with targeted therapies to improve tolerance, reduce irritability, and restore full function.
The goal isn’t to “treat the tendon” in isolation. It’s to improve its capacity, reduce excessive stress, and address the factors that caused overload in the first place.
Here’s how that typically looks.
1. Progressive Strengthening (Built on Evidence-Based Loading Principles)
Our Doctor of Physical Therapy trained physical therapist will create a plan to help you fully strengthen your achillies tendon. Learn more about physical therapy at Boulder Sports Clinic.
Strengthening follows the key principles discussed above:
- 70–90% of 1RM when appropriate
- ~6 seconds per repetition (3 up, 3 down)
- Gradual progression from isometrics → heavy slow resistance → plyometrics
- Pain-monitored loading (≤5/10 during exercise, no next-day flare)
In early-stage or highly irritable tendons, we may begin with isometric calf holds to calm pain while maintaining load exposure.
As tolerance improves, we transition into:
- Weighted single-leg heel raises
- Seated calf raises (to bias soleus)
- Semi-stiff deadlifts
- Later-stage hopping and bounding drills
The objective is not just pain reduction — it’s restoring true load capacity, especially for runners and field athletes in Boulder who return to hills, trails, and high mileage.
2. Shockwave Therapy
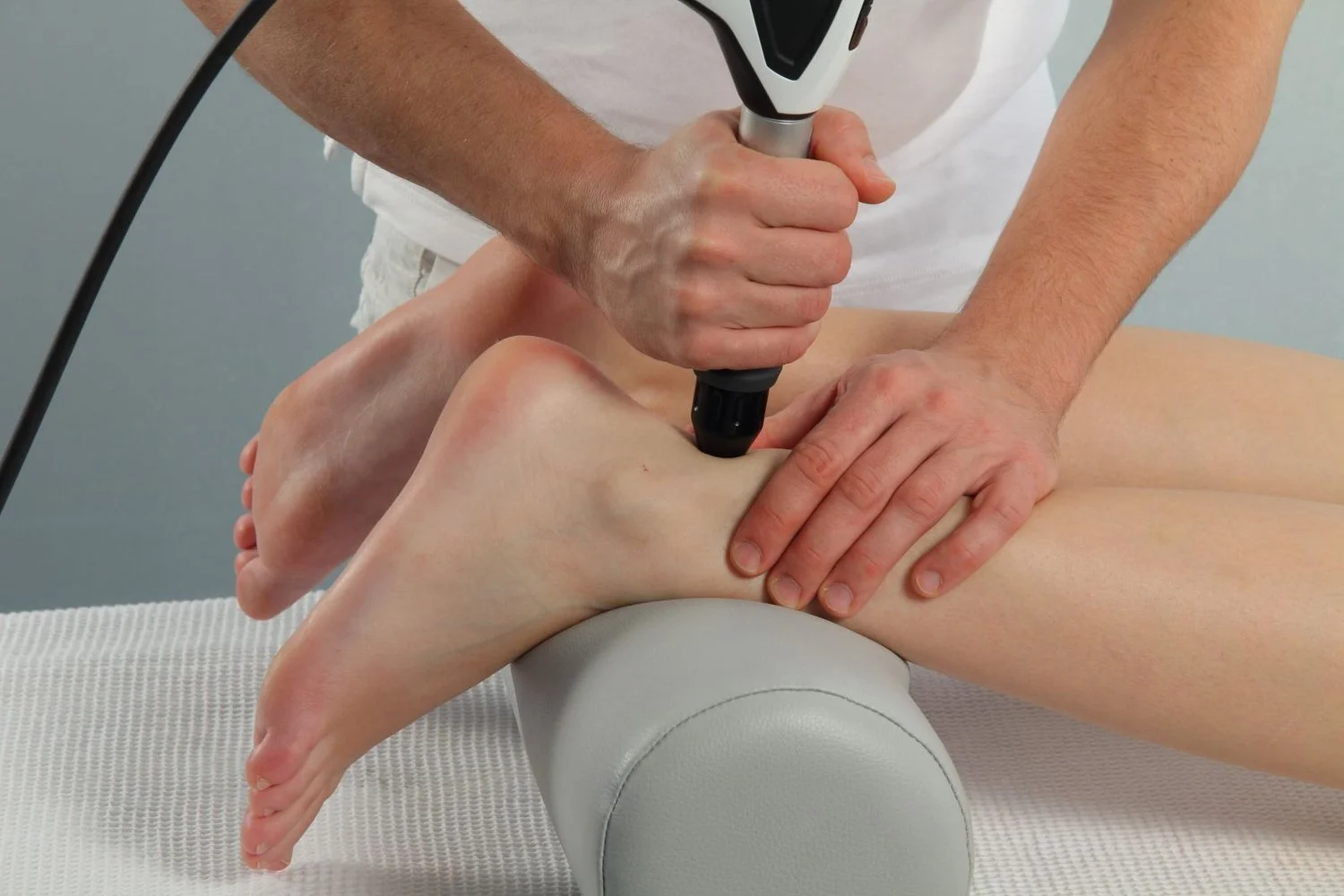
Shockwave therapy (ESWT) is often helpful for chronic or stubborn Achilles tendinopathy.
It may:
- Stimulate local blood flow
- Promote tendon remodeling
- Reduce persistent pain sensitivity
Shockwave does not replace loading — it supports it.
We typically use it in combination with progressive strengthening, especially in cases that have plateaued after months of basic rehab. To learn more about shockwave therapy, click here.
3. Dry Needling
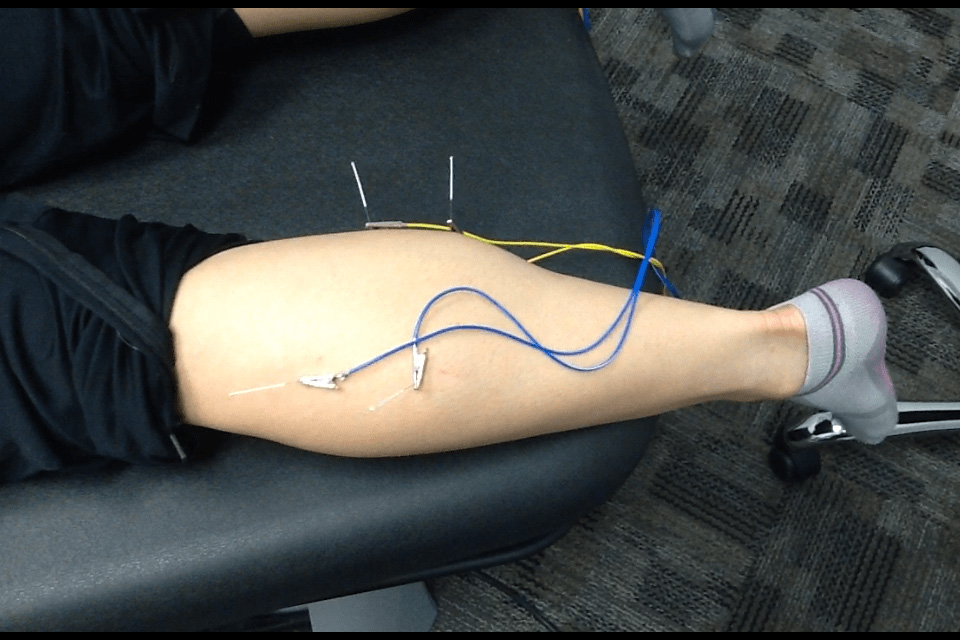
Calf muscle stiffness often increases tendon strain.
Dry needling may be used to:
- Reduce myofascial trigger points in the gastrocnemius or soleus
- Improve ankle mobility
- Decrease protective muscle guarding
In some cases, electrical stimulation is applied to needles to enhance neuromuscular activation.
Again, this is supportive care — it improves the environment around the tendon so strengthening is better tolerated. To learn more about dry needling in boulder, click here.
4. Class IV Laser Therapy

Laser therapy may help:
- Improve circulation
- Reduce inflammatory signaling
- Support tissue healing in irritated tendons
We most often use laser during more reactive or painful stages to help patients tolerate loading more comfortably. To learn more about class 4 laser therapy in boulder, click here.
5. Run Gait Analysis for Runners

To see a video demonstration of our gait analysis, check it out on youtube by clicking here.
For runners, Achilles tendinopathy is often a load management issue, not just a tissue issue.
We evaluate:
- Cadence (low cadence increases tendon load)
- Overstriding
- Excessive vertical oscillation
- Foot strike patterns
- Ankle stiffness and push-off mechanics
- Training volume and terrain changes
Often, small adjustments — such as increasing cadence by 5–7% — can significantly reduce Achilles strain.
In Boulder, where trail running and hill training are common, terrain plays a major role. Downhill and steep climbing can increase tendon stress dramatically.
Rehab for runners typically includes:
- Controlled return-to-run progressions
- Hill exposure management
- Plyometric progression before full mileage return
Why We Combine These Approaches
Exercise drives tendon adaptation.
Manual therapies and advanced modalities improve tolerance and accelerate progress.
Our approach is typically:
- Calm excessive irritability (if present)
- Build progressive tendon capacity using heavy slow resistance
- Correct contributing biomechanical factors
- Gradually reintroduce sport-specific loading
Not every patient needs every modality. The treatment plan depends on:
- Irritability level
- Chronicity
- Training demands
- Strength deficits
- Response to loading
The Bigger Picture
Achilles tendinopathy is rarely solved by passive care alone — and it’s rarely solved by random exercises either.
The most consistent outcomes occur when:
- Loading intensity is appropriate
- Tempo is controlled
- Volume is progressed systematically
- Biomechanics are addressed
- Return to sport is staged thoughtfully
If Achilles pain keeps returning despite stretching and basic heel raises, it usually means one of those variables hasn’t been optimized yet.
Common Mistakes We See
- Staying at bodyweight too long
- Moving too fast during reps
- Skipping strength progression
- Jumping back into plyometrics too soon
- Ignoring insertional range limitations
Most chronic Achilles cases improve when loading is structured properly.
The Bottom Line
Achilles tendinopathy rehab isn’t about “just doing heel raises.”
It’s about:
- Loading heavy enough (70–90% 1RM)
- Moving slow (~6 seconds per rep)
- Progressing volume appropriately
- Incorporating multiple contraction types
- Tailoring the plan to the individual
Tendons adapt to the loads placed upon them. The key is placing the right load at the right time.
If you’re unsure how to progress your Achilles rehab — especially if pain keeps returning — a structured evaluation can help clarify what stage you’re in and what variable needs adjusting.
Frequently Asked Questions About Achilles Tendinopathy
1. What is the fastest way to heal Achilles tendinopathy?
There is rarely a “fast” fix. The most effective treatment is progressive, heavy loading of the tendon using structured strengthening. Shockwave therapy, laser therapy, and dry needling may help reduce pain and improve tolerance, but exercise is the foundation of recovery.
2. Should I rest completely if my Achilles hurts?
Complete rest is usually not recommended. Tendons require mechanical loading to remodel and become stronger. Relative load management — reducing aggravating activity while maintaining controlled strengthening — is typically more effective than full rest.
3. Are eccentric heel drops still recommended?
Yes, but they are not the only option. Research now supports using isometric, concentric-eccentric (heavy slow resistance), and plyometric loading depending on the stage of rehab. The key factor is progressive load — not just eccentric-only exercises.
4. Does shockwave therapy work for Achilles tendinopathy?
Shockwave therapy has moderate evidence supporting its use in chronic Achilles tendinopathy. It may stimulate local healing and reduce persistent pain sensitivity. It is most effective when combined with progressive strengthening.
5. Is dry needling helpful for Achilles pain?
Dry needling does not directly repair the tendon, but it can reduce calf muscle tightness and improve mobility. This may decrease strain on the Achilles and make strengthening exercises more tolerable.
6. How long does Achilles tendinopathy take to heal?
Most cases improve in 8–12 weeks with consistent, progressive loading. Chronic cases may take longer. Recovery time depends on tendon irritability, duration of symptoms, and how well loading is structured.
7. Can I keep running with Achilles tendinopathy?
Often, yes — with modifications. We typically adjust volume, reduce hills, increase cadence slightly, and implement a structured return-to-run plan. Run gait analysis helps identify biomechanical contributors to excessive tendon load.
8. What is the difference between insertional and midportion Achilles tendinopathy?
Midportion pain occurs 2–6 cm above the heel bone. Insertional pain occurs directly at the heel attachment. Insertional cases require limiting excessive dorsiflexion early in rehab to reduce compressive stress.
About the Author
Dr. Steve Brown, DC
Chiropractor | Co-Owner, Boulder Sports Clinic
Dr. Steve Brown is a chiropractor and co-owner of Boulder Sports Clinic in Boulder, Colorado. He has over 13 years of experience treating athletes and active adults, from professional competitors and collegiate teams to runners, lifters, and weekend warriors.
He focuses on evidence-based management of running injuries, tendon conditions, and performance-related pain. His approach combines progressive loading principles, biomechanical assessment, chiropractic care, and advanced therapies such as shockwave therapy, laser therapy, and dry needling when appropriate.
Dr. Brown works closely with the clinic’s physical therapy team to help patients move beyond pain relief and return confidently to sport and activity.
To schedule your appointment, click here.
Related Posts

The Right Shoe for Injury Recovery and Prevention: A Guide to Healthy Feet

The Best Over-the-Counter Pain Relief Options for Neck & Back Pain
.JPG)
Shockwave Therapy Near Me – Boulder, CO
Experience the difference at Boulder Sports Clinic.
Contact us today to schedule an appointment and start your journey towards optimal health and peak performance. Still have questions? Call us now at (303) 444-5105

